Antibiotic resistance
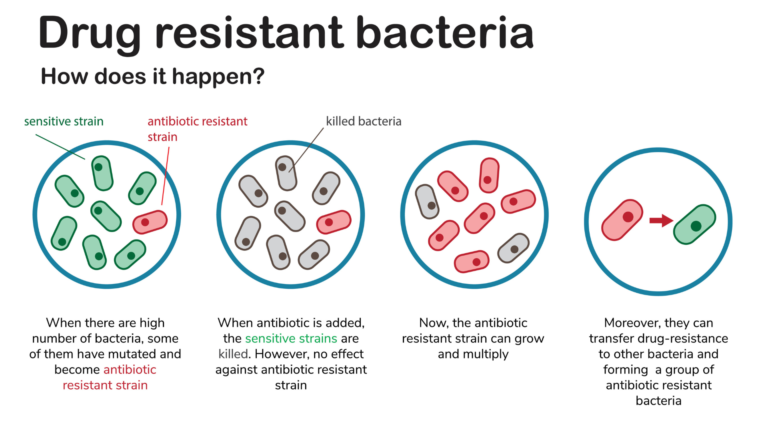
Antibiotic resistance is when a bacterium or fungus becomes resistant to antibiotics. This resistance can be developed when microbes are exposed to antibiotics. This antibiotic resistance can be transmitted and spread between pathogenic bacteria, bacteria on our body and bacteria in the environment. Overuse and often incorrect use are the main reasons for the spread of the phenomenon. This phenomenon is often called « The invisible epidemic »
In France, there are over 150,000 infections per year with multi-drug resistant bacteria, resulting in the death of 12,500 patients. This figure increases to more than 33,000 patients in Europe.
Covid-19 has even accelerated and worsened the phenomenon; according to the Center for Disease Control and Prevention, in the first year of the pandemic more than 29,400 people died as a result of infections associated with multi-antibiotic resistant bacteria.
In the first year of the pandemic, more than 80% of patients hospitalised for covid received an antibiotic. Antibiotic resistance is one of the most serious threats to global health, as well as being a socio-economic problem.
Sources:
https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(21)02724-0/fulltext
https://solidarites-sante.gouv.fr/IMG/pdf/o_neill_3_final_report_.pdf
OMS, Santé Publique France and European Centre for Disease Control and Prevention (ECDC)
Our solutions can have an impact on the United Nations Sustainable Development Goal (SDG) 3.d.2: percentage of bloodstream infections due to selected antimicrobial-resistant organisms.
In 2015, 671,689 cases of infections with antibiotic-resistant bacteria were recorded in the European Union.
According to the Organisation for Economic Co-operation and Development (OECD): 2.4 million people could die from an infection caused by an antibiotic-resistant microbe in Europe, North America, and Australia between 2015 and 20502.
Antibiotic resistance will cost the health services of 33 OECD countries an estimated US$ 3.5 billion per year.

Disclaimer: Funded by the European Union. Views and opinions expressed are however those of the author(s) only and do not necessarily reflect those of the European Union or the Directorate-General for Communications Networks, Content and Technology. Neither the European Union nor the granting authority can be held responsible for them.
