Biofilms
Biofilm : a term first introduced in 1978 to refer to a community of thousands to millions of microorganisms embedded in an extracellular polymer-rich matrix and in contact with a surface. It was soon realised that biofilm is the preferred way of life for microorganisms.
Biofilms can form on any surface and are often the source of nosocomial infections. They can also form in minutes or hours and last for years.
Many bacteria and fungi can form biofilms, however, other microorganisms (i.e. viruses, yeast, other pathogenic bacteria) can embed themselves and take advantage of the protective matrix and its humid environment and thus result in the formation of polymicrobial biofilms.
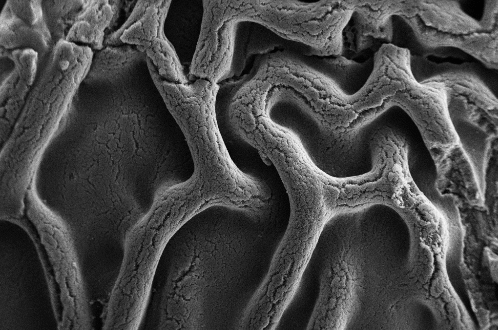
Skander Hathroubi
In addition to keeping the microorganisms within the biofilm, the matrix represents a real physical and chemical barrier. In fact this dense network of polymers of all kinds strongly limits the penetration and diffusion of biocides, thus limiting their effectiveness. Microorganisms inside a biofilm are 10 to 1000 times more resistant and tolerant to biocides.
According to an estimate by the National Institute of Health (NIH, USA), approximately 60-70% of all hospital-acquired infections are caused by biofilms.
They are intimately linked to implants such as central venous and urinary catheters.
In the US, out of every 5 million medical devices or implants used per year, 1 to 6% become infected. For pacemakers/defibrillators alone, within 12 months of transplantation, 1-3% will develop a biofilm. Considering more than one million pacemakers are implanted each year worldwide, the global cost for this type of infection is estimated to be more than $220 million.
Sources :
Malone, M. et al. The prevalence of biofilms in chronic wounds: a systematic review and meta-analysis of published data. J. Wound Care 26, 20–25 (2017). https://pubmed.ncbi.nlm.nih.gov/28103163/
Cámara, M., Green, W., MacPhee, C.E. et al. Economic significance of biofilms: a multidisciplinary and cross-sectoral challenge. npj Biofilms Microbiome@42 (2022). https://doi.org/10.1038/s41522-022-00306-y

Disclaimer: Funded by the European Union. Views and opinions expressed are however those of the author(s) only and do not necessarily reflect those of the European Union or the Directorate-General for Communications Networks, Content and Technology. Neither the European Union nor the granting authority can be held responsible for them.
