Antibiotic resistance, is defined as the ability of a bacterium to become insensitive to the action of one or more antibiotics.
This phenomenon is the result of repeated exposure to antibiotics. When many bacteria survive more than one class of antibiotic, it is called multidrug resistance. It calls into question the effectiveness of available treatments and can represent a threat to human and animal health. Antibiotic resistance is a global concern.
Antibiotic resistant bacteria are therefore a public health issue. In health establishments, the most frequently encountered resistant bacteria are Staphylococcus aureus and enterobacteria, which are responsible for serious nosocomial infections. They have been the subject of a surveillance and prevention programme since the 1990s.
In the city, antibiotic resistance is also observed, particularly in pneumococci (Streptococcus pneumoniae).
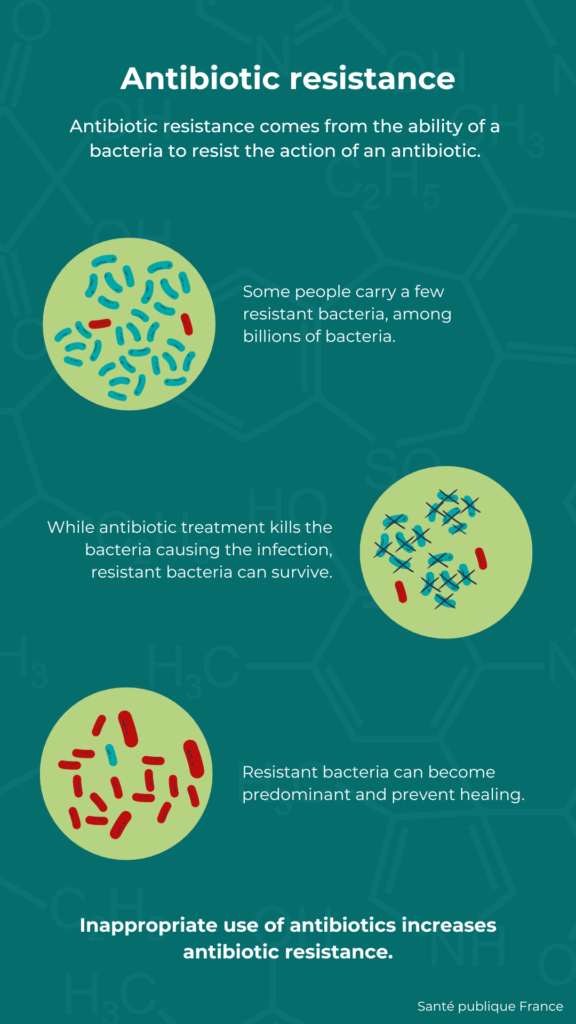
Bacteria can escape the action of an antibiotic due to a genetic mutation, either spontaneous or encouraged by exposure to antibiotics. The resistance is then written into its genes. As the bacteria multiply, they will pass on their antibiotic resistance to subsequent generations of bacteria through replication.
More often, resistance mechanisms are passed on through DNA from one bacterium to another. It is through this mechanism that a resistance that appears in a bacterium in the environment or that infects an animal can be transmitted to a bacterium that infects humans.
The WHO has published recommendations on how to limit antibiotic resistance.
SPARTHA Medical’s innovation is unequalled because it has an antibacterial effect without the use of antibiotics.
It is derived from natural polymers, making it biocompatible, and is applicable to all types of surfaces. These nano/microscopic coatings can protect medical devices from bacterial infection, including antibiotic-resistant strains, without affecting their primary function.
While antibiotic resistance is a well-studied phenomenon in humans and animals, it can also be caused by the release of antibiotics intoterrestrial and aquatic environments. These nano/microscopic coatings can protect medical devices from bacterial infection, including antibiotic-resistant strains, without affecting their primary function.
